
At OTC Benefits Program, we strive to make administering an OTC Supplemental Benefit simple. Below are some Frequently Asked Questions to give you a better understanding of how our OTC Benefit Program can fit into any Health Plan.
Question: How long does it take to set up a Supplemental OTC Benefit with OTC Benefits Program?
Answer: We generally request a minimum of 3 months to start date to give us time to build your custom branded website, catalog, sufficiently stock our warehouse, and develop call scripting for our Call Center. Learn more about How the Program Works here.
Setup Timeline
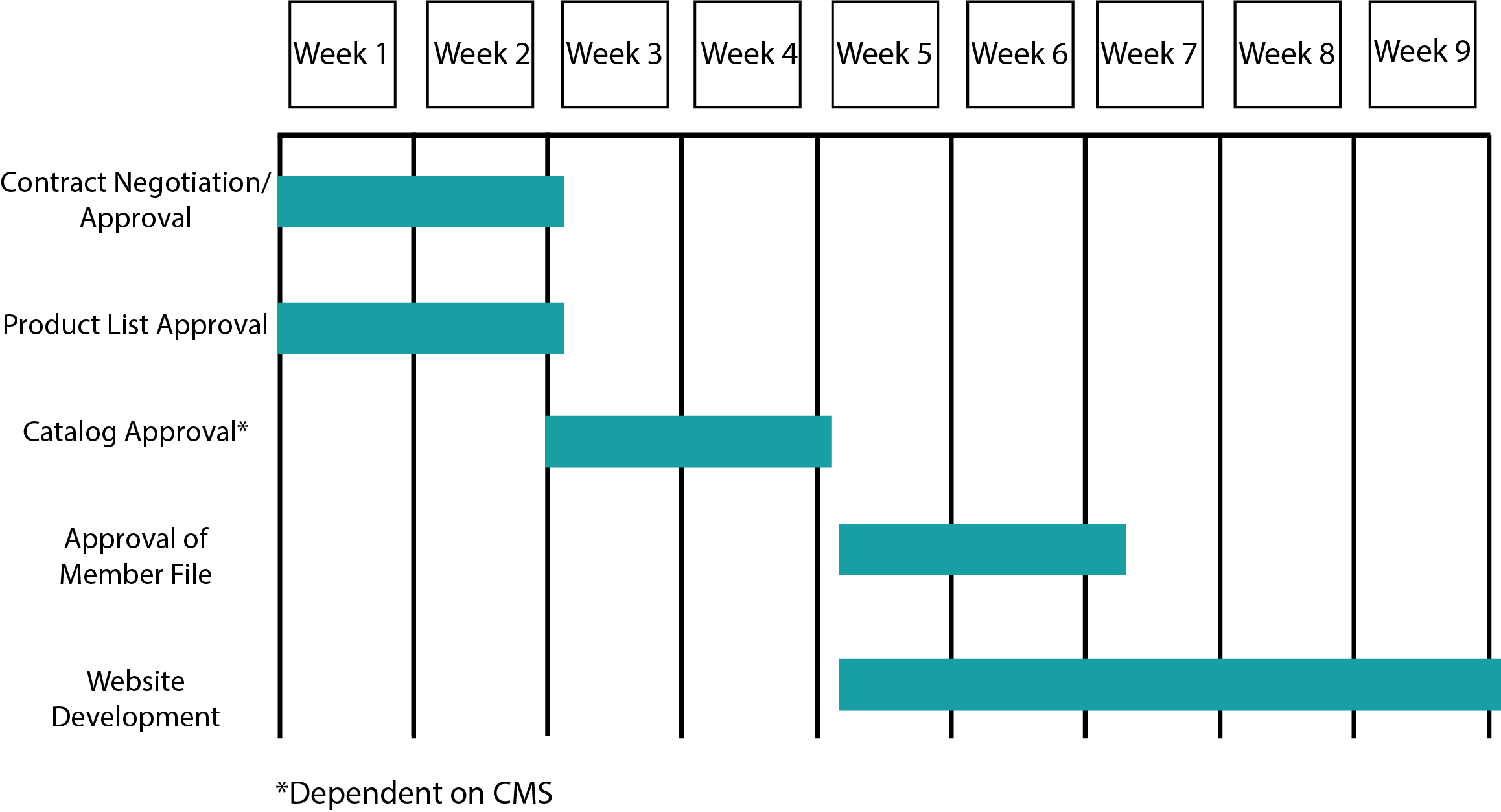
What is the standard OTC benefit frequency?
We have worked with Medicare Advantage Plans that offer a variety of different benefit frequencies, granting us insight into the frequencies that generate the most utilization: $80 per quarter or $25 per month. However, due to our flexible and scalable OTC Mail Order Catalog Programs, we are able to offer any amount at any frequency the Health Plan requests.
How are the OTC product lists developed?
Keeping an eye on trends in the OTC market – and keeping CMS product guidelines in mind – we work closely with the Health Plans to determine their custom eligible and dual purpose product catalog. The OTC Benefit amount can limit the inclusion of more expensive products, but we present Plans with a list from which they are able to pick and choose what generic and brand name products they want to include. We develop fair custom pricing based on factors such as member population, location, utilization, and freight.
Can the benefit roll over and accumulate from benefit cycle to benefit cycle?
Yes it can. We offer rollover options for our programs, as well as benefits that expire at the end of the cycle if not spent.
Can a member exceed their benefit amount?
Our OTC Benefit Program includes credit card processing capabilities as an option for members who want to exceed their benefit amount. These are only included at the Health Plans request. If there is no credit card option, the member cannot overspend.
How many orders can a member place per benefit period?
Members can place as many orders as they want per period unless the Health Plan instructs otherwise. OTC Benefit Solutions generally recommends limiting members to one shipment per benefit cycle – this keeps shipping costs lower for the Health Plan.
How quickly are orders processed?
We process orders at our Fulfillment Center within a 24-48 hour window of receiving them, and members receive shipments in 3-7 days based on member location.
How does OTC Benefits Program handle secure member data?
OTC Benefits Program utilizes a File Schema to efficiently layout your eligibility data for import. This is easily generated by your IT teams. Data is transferred via an encrypted SFTP site. We utilize a state-of-the-art secure hosting facility, specializing in HIPAA compliance. All internal data is password protected for access by authorized personnel only. Data is retained internally on hardware-encrypted disk drives. Staff are HIPAA, HITECH trained on a yearly basis. Learn more about our data security here.
Didn’t find your answer?
We’d be more than happy to answer any questions you may have, or provide you with a free OTC Benefit Program quote, just contact us.
